Gastric Band Surgery: How It Works and Why It Supports Long-Term Weight Loss
Gastric band surgery is a proven weight loss treatment for people living with obesity. Many people explore gastric band surgery when diet and exercise alone have not delivered lasting results. The procedure reduces stomach capacity and helps control hunger. As a result, patients often feel satisfied after eating much smaller meals.
Doctors classify gastric band surgery as bariatric surgery. Specialists designed these procedures to support long-term weight loss and improve obesity-related health conditions. Many people experience improvements in type 2 diabetes, blood pressure, and mobility after surgery. Success depends on commitment, guidance, and the right medical support.
Understanding how gastric band surgery works helps people make confident decisions. The process sounds complex at first. However, the concept remains simple. A small adjustment to the stomach can transform how a person eats and feels about food.
How does it work?
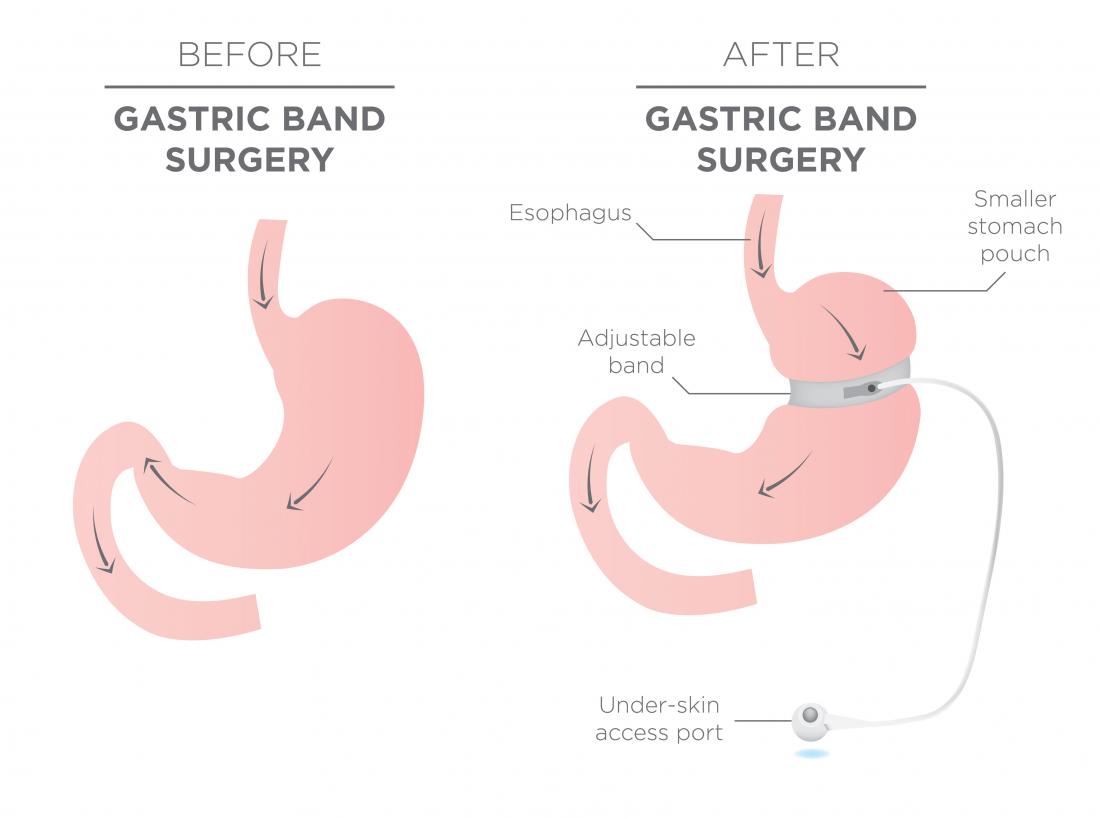
How Gastric Band Surgery Works
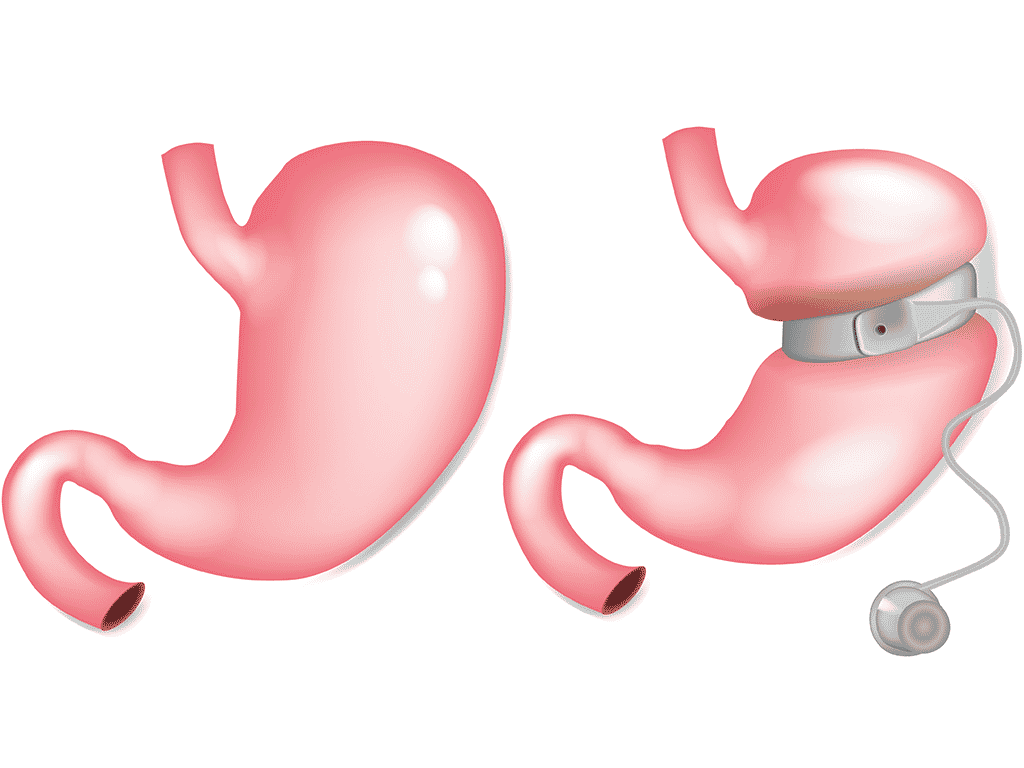
Gastric band surgery works by reducing the amount of food the stomach can comfortably hold. Surgeons place a soft silicone band around the upper part of the stomach. This band creates a small pouch above the rest of the stomach.
Food enters this small pouch first. The pouch fills quickly during meals. Because of this, the brain receives fullness signals much sooner. Patients feel satisfied after eating far less food.
The procedure also slows how quickly food moves through the stomach. Meals pass gradually from the pouch into the lower stomach. That slower movement helps people stay full for longer.
A thin tube connects the band to a small port placed beneath the skin of the abdomen. Doctors access this port using a fine needle. They inject or remove saline fluid to adjust the band.
Adding saline tightens the band slightly. Removing saline loosens it. These adjustments control how quickly food passes through the stomach opening.
Adjustments form a key part of gastric band surgery. Specialists personalise the band tightness for each patient. The aim involves finding the balance between comfortable eating and effective weight loss.
A Minimally Invasive Bariatric Procedure
Many people choose gastric band surgery because the procedure is less invasive than other bariatric operations. Surgeons perform the surgery using laparoscopic techniques. Small incisions replace the need for large surgical cuts.
This keyhole approach offers several advantages. Patients usually experience less pain after surgery. Recovery time also tends to be quicker. Many patients return home the same day or the following morning.
Another important benefit involves reversibility. Surgeons can remove the gastric band if medical needs change later. The stomach returns to its original shape once the band is removed.
Unlike some other weight loss procedures, gastric band surgery does not permanently alter the digestive system. Food continues to pass through the stomach and intestines normally. The body still absorbs nutrients in the usual way.
This feature appeals to many people considering bariatric surgery. They prefer a procedure that supports weight loss without affecting digestion or vitamin absorption.
Life After Gastric Band Surgery
Recovery after gastric band surgery requires patience and commitment. Doctors recommend a carefully structured diet during the early healing stage. The stomach needs time to adapt to the new band placement.
Patients begin with a liquids-only diet. This stage usually lasts around one to two weeks. Liquids protect the stomach while swelling reduces after surgery.
Gradually, patients move to soft foods. This stage often continues for several weeks. Foods such as yoghurt, soups, and puréed meals work well during this phase.
Solid foods return slowly as healing progresses. Most patients follow a staged diet plan lasting about six weeks.
Eating habits change significantly after surgery. Patients learn to eat slowly and chew thoroughly. Small bites become essential. Large bites may cause discomfort or pressure in the stomach pouch.
Drinking habits also change. Doctors advise avoiding fluids during meals. Liquids can push food through the pouch too quickly. Waiting thirty minutes before or after meals helps maintain fullness.
These changes support the success of gastric band surgery. They also help patients build healthier eating behaviours for the long term.
The Role of Gastric Band Adjustments
Adjustments play an important role in gastric band success. After surgery, the band usually starts fairly loose. This allows the stomach to heal comfortably.
Several weeks later, specialists perform the first adjustment. They inject a small amount of saline into the port beneath the skin. The saline tightens the band slightly.
Patients often require several adjustments during the first year. Each adjustment fine-tunes the restriction level. The goal involves reducing hunger while allowing comfortable eating.
Many patients describe adjustments as quick and straightforward. Clinicians usually complete the process during a short clinic appointment. The procedure takes only a few minutes.
Adjustments help maintain steady weight loss. They also support long-term weight management. Without adjustments, the band cannot provide its full benefit.
Regular follow-up appointments therefore remain essential. These visits allow specialists to monitor progress and make necessary changes.
Weight Loss Results After Gastric Band Surgery
Weight loss after gastric band surgery varies between individuals. Many patients lose weight gradually over twelve to twenty-four months. Slow and steady progress often leads to better long-term success.
Patients typically lose between 40 and 60 percent of their excess body weight. However, results depend heavily on lifestyle habits. Surgery provides a powerful tool. Healthy behaviours unlock its full potential.
Smaller meals become easier to maintain after surgery. Cravings often reduce because the stomach fills quickly. Patients also report feeling satisfied for longer periods between meals.
Physical activity also plays an important role. Regular movement supports calorie balance and overall health. Walking, swimming, and cycling provide excellent starting points for many patients.
Support networks also improve outcomes. Guidance from bariatric professionals helps patients navigate the adjustment process. Ongoing support often increases long-term success.
Health Improvements Beyond Weight Loss
Weight loss forms the primary goal of gastric band surgery. However, many patients also experience improvements in overall health. Carrying less weight reduces strain on many body systems.
Several obesity-related conditions often improve after surgery. Type 2 diabetes may become easier to manage. Blood sugar levels often improve as weight decreases.
Blood pressure frequently reduces as well. Lower blood pressure decreases the risk of heart disease and stroke.
Joint pain also improves for many patients. Less weight places reduced stress on knees, hips, and the lower back. Many patients report improved mobility within months of surgery.
Sleep quality may also improve. Some people experience relief from sleep apnoea symptoms after losing weight.
These health improvements often provide strong motivation for patients. Weight loss becomes part of a wider journey towards better wellbeing.
Who May Be Suitable for Gastric Band Surgery
Doctors assess several factors when considering gastric band surgery. The procedure usually suits people with a body mass index above 40. Patients with a BMI above 35 may also qualify if obesity causes related health conditions.
Lifestyle commitment also matters. Gastric band surgery requires long-term dietary changes and regular follow-up care. Patients must attend adjustment appointments and follow medical advice carefully.
Healthcare providers also assess emotional readiness. Surgery supports weight loss, but it cannot replace lifestyle habits. Patients must feel prepared to change how they eat and live.
In the UK, bariatric surgery often follows guidance from NHS eligibility criteria. Many people explore private options when waiting times remain long. Private clinics may offer faster access to surgery and follow-up care.
Specialist advice helps determine the best option for each person. A full consultation usually includes medical history, weight history, and lifestyle discussion.
Long-Term Success with Gastric Band Surgery
Long-term success depends on partnership between patient and healthcare team. Surgery provides the starting point. Daily habits shape the outcome.
Regular follow-up appointments help maintain progress. Adjustments ensure the band continues working effectively. Specialists also monitor weight changes and overall health.
Healthy eating patterns remain essential. Balanced meals support steady weight loss and good nutrition. Protein-rich foods often form the foundation of post-surgery diets.
Hydration also remains important. Drinking enough water supports digestion and overall wellbeing. However, patients must remember to separate drinking from meals.
Emotional support also matters. Many patients benefit from support groups or counselling during their weight loss journey. Sharing experiences often builds motivation and confidence.
Over time, many people find that gastric band surgery transforms their relationship with food. Meals become smaller but more satisfying. Energy levels improve and confidence often grows.
A Tool for Long-Term Weight Management
Gastric band surgery offers a structured approach to weight loss. The procedure supports portion control and reduces hunger. Patients feel full sooner and eat less without constant struggle.
The adjustable nature of the band makes it highly adaptable. Doctors can refine the restriction level over time. This flexibility helps maintain progress during different life stages.
Success does not happen overnight. Weight loss occurs gradually. However, steady progress often leads to sustainable results.
Many patients view gastric band surgery as the beginning of a new chapter. With the right guidance and commitment, the procedure can support lasting weight control and improved health.